By Mary Meehan
Ohio Valley Resource
Sitting on top of the Bible on Pastor Brad Epperson’s desk at the Clay City First Church of God is a list of goals for his small congregation written in a looping cursive hand.
“Our community ought to see the love of God in us, not just by our understanding of a compassionate Gospel, but our public acts of love,” is near the top.
Epperson was born and raised in Powell County in the mountains of eastern Kentucky.
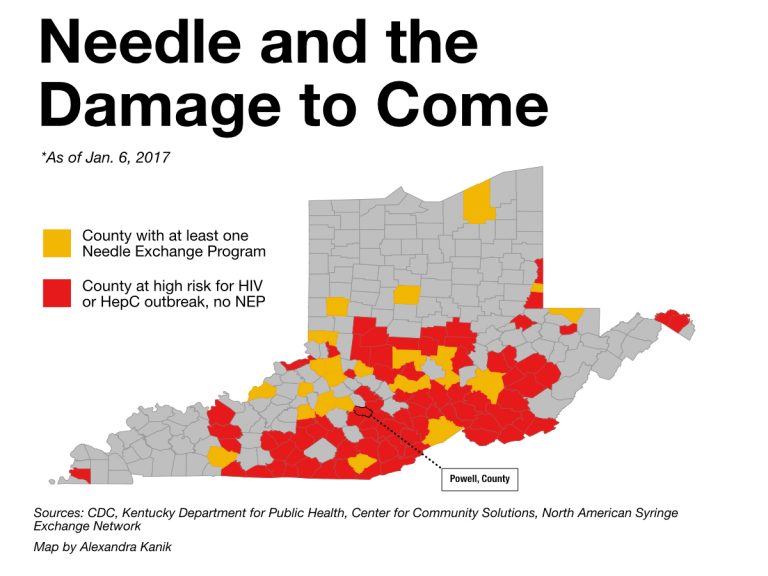
It is one of nearly 100 counties in Kentucky, Ohio, and West Virginia designated at high risk for HIV infection by the Centers for Disease Control and Prevention. The 10 counties the CDC identified as highest risk are all in eastern Kentucky and southern West Virginia. Powell County ranks 15th in the nation. Wolfe County, next door, ranks a sad number one.
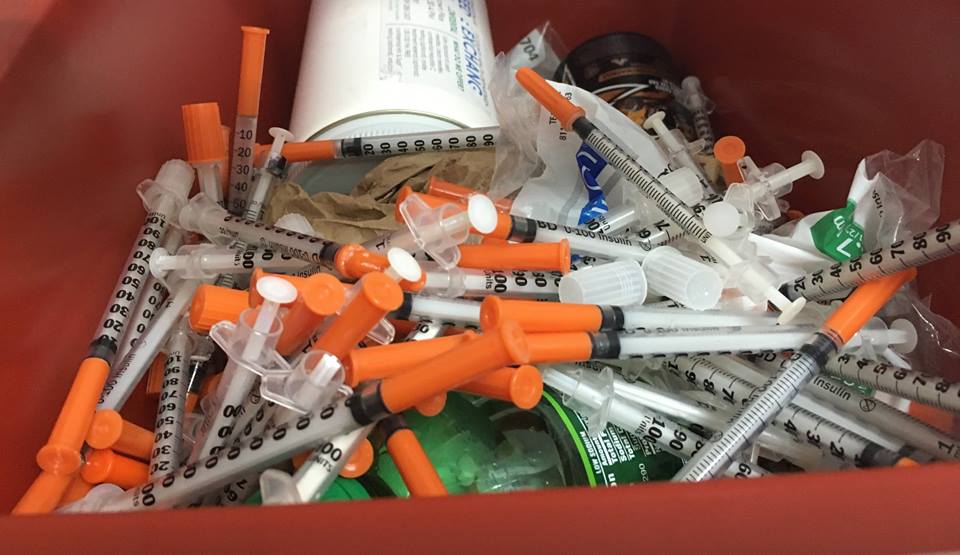
In the first year of operation the Lexington – Fayette County Health Department collected 20,199 needles and distributed, 21,693
That means Epperson and his community are at the epicenter of the heroin-related public health crisis that is ravaging rural America. And addressing that threat would force Epperson and many others in this religious, conservative community to take a hard look at themselves and their deeply held convictions.
A Tough Decision
Epperson moved away for a more than a decade to tend a church in Tennessee. When he came to Clay City a few years ago he didn’t recognize the place. The impact of drug addiction was everywhere. At the Clay City First Church of God, the first brick building in town after exiting the Mountain Parkway, he conducted too many funerals for people way too young.
Epperson, who is also a school bus driver, saw the pain in the lives of the kids he carries. One boy excitedly told him that both his parents were going to be out of jail at the same time for Christmas. No child, Epperson said, should have that kind of life.
Epperson said he struggles with how to help addicts without appearing to condone drug abuse. He sees addiction as a disease with a moral underpinning. First, there is the collateral damage. Cancer patients don’t steal from Mammaw to pay for chemo. Diabetics don’t infect their spouses.

Pastor Brad Epperson had to reconsider his own views about addiction as a moral issue before he could commit to support a needle exchange program. (Photo by Mary Meehan/Ohio Valley ReSource)
Second, he said, addicts make the choice to take in that first drug.
Still, he knew something had to change.
Others in his community were having their own struggles.
Six months ago, Mandy Watson, a nurse at the Powell County Board of Health, couldn’t imagine a needle exchange program in her hometown.
“When it first started I actually called several of my friends and told them, ‘Pray that this will not happen here,’” she said.
But then Watson saw the projected devastation if her small community had an HIV outbreak. She listened to the statistics about how infection rates could be lessened. She said she couldn’t cure the addict, but she could help someone to be just a little bit safer. That could help stop the spread to innocents in the community such as a spouse unaware of needle use, or kids at a playground where users stash dirty syringes.
She had to do something.
“We are all very close, we all know each other here,” she said, “and the thought of knowing that Hep C and HIV outbreaks could happen very easily here, it scared me for not only my child but my friends’ children. Almost anybody you ask has some kind family member who does use or some type of trouble with addiction.”
Physician Assistant Troy Brooks is on the Powell County Board of Health. He, like Watson, was against needle exchanges. He said it seemed like a way to let addicts keep using their drug of choice without consequence.
A deciding factor for him was that local police, whose job increasingly involves confiscating or collecting needles, could be better protected if fewer dirty needles were in circulation. He has a friend who fears infection from an inadvertent stick. His only recourse is to keep dirty needles in a plastic water bottle in his squad car.
That same officer showed him how widespread the problem really ways.
“He went out to the Clay City playground, I think he collected 41 needles that had been stashed in different places around the playground. That put me over the edge,” Brooks said.
Having each changed their mind, the trio sought to help change the minds of others. Last fall, the Powell County Fiscal Court, the Powell County Board of Health, and the Stanton City Council all unanimously approved the creation of the needle exchange program. Watson hopes to have it up and running by the end of January.
A Fundamental Change
The head of the Kentucky Office of Drug Control Policy, Van Ingram, said that’s not a surprise. Conservative, rural counties like Powell are at the forefront of a sea change in how addiction is perceived. He said there’s a fundamental shifting toward viewing drug abuse as an illness rather than a crime, taking it primarily out of the hands of the criminal justice system and framing it more as a public health crisis.

Powell County Public Health Nurse Mandy Watson first prayed to stop a needle exchange program. But concern about an HIV outbreak changed her mind (Phto by Mary Meehan/Ohio Valley ReSource)
“There is a movement in this state and a lot of other states to do some things differently, ” he said.
In West Virginia, Wheeling-Ohio County Health Department Administrator Howard Gamble said what exactly happens at a needle exchange, such as specific hours or additional services, varies from place to place. But he said the important thing is for communities to take action. “No one is doing it wrong,” he said, so long as they are making an effort.
But as Powell County’s experience shows, it can be difficult.
A Shocking Outbreak
Following a spring 2015 HIV outbreak of nearly 200 in Austin, Indiana, population, 4,200, legislatures in Ohio, West Virginia and Kentucky scrambled to pass laws allowing health departments to create needle exchange programs by local ordinance.
Exchange programs, which started in the 1980s in Amsterdam, have been proven to reduce rates of HIV and Hepatitis C infection and help connect addicts with treatment.
But there are long-standing misconceptions.
“There are a lot of assumptions about the clients who use our program, that they are violent, that they are dangerous,” said Lynnsey McGarrh, who has the title needle exchanger at the Lexington-Fayette County Health Department.

(By Alexandra Kanik)
McGarrh said Fayette County was one of the first places in Kentucky to enact a needle exchange program and after a year in operation and there have not been issues of violence. In fact, she said, they are generally very grateful.
The program has also collected 20,199 needles and given out 21,693. They also provide the anti-overdose drug Naloxone, testing for HIV and Hepatitis C, and treatment referrals.
“Nobody grows up hoping to become an addict,” said McGarrh, who admits to sometimes crying with her clients as they struggle to get well.
McGarrh said the key to the program is for the active user to have someone like her willing to help, not judge.
“I’ll Keep Coming Back”
That’s the kind of compassion that has kept Allie, who asked not to be identified by her last name, coming to the Lexington needle exchange. Dressed in a black North Face jacket and black leggings, she looks like a student. At 24, she has been injecting heroin off and on for four years. She’s been a client at the Lexington-Fayette County Health Department for about six months. She was clean for nearly a year but relapsed, losing her job as a waitress. For a while she lived in her car.
But even in active addiction, she managed to get to the Fayette County needle exchange during its small window of operation from 11 a.m. to 4:30 on Fridays to get clean needles. She felt helpless over a lot of things in her life, she said, but she could do this one thing to help herself.
Last fall, when she was still a little high from using earlier in the day, Allie got back some test results.
“Well at first, the first few weeks I came I wasn’t sure that I was, that I had Hep C yet. But I actually just got the test done and it came back positive, so I just found that out five minutes ago,” she said, still a bit dazed from the news.
Click here for a list of Needle Exchange Programs in Kentucky, Ohio and West Virginia
She knows there is medical treatment, but the fear is clear in her eyes. She’ll keep coming back to the health department. Her 15 minutes a week while she exchanges needles is a respite from the chaos of her life. The staff members listen, she said. “They don’t try to change me, they don’t judge me.”
Most of her family and friends have disowned her because of her addiction.
“Can’t Give Up”
For Pastor Epperson, needle exchange programs are the beginning of the outreach. There has to be physical healing and avoidance of disease. But he said that must be coupled with moral support and spiritual outreach.
“They are made in the image of God, they’re highly redeemable. I believe that with all my heart. I don’t think we can stand by and say, ‘Well, we are going to give up on them,’” he said
.

Physician Assistant Troy Brooks decided to support a needle exchange program, in part, because it helps protect law enforcement and others in the community from getting exposed to dirty needles. (Photo by Mary Meehan/Ohio Valley ReSource)
Ingram, who heads the Kentucky Office of Drug Control Policy, said the change in Powell County can happen in other communities. People, he said, “have to be met where they are.” Questions of faith and science have to be answered with equal openness and seriousness, he said.
Local folks have to bring the conversation to their networks of friends and family. In Powell County, Brooks, the Physician Assistant; Epperson, the pastor; Watson, the nurse — they all went to school together.
The trio had support in their community outreach from Kevin Hall, spokesman for the Fayette County Health Department. He provided a template based on how the Fayette County program works and helped make presentations to Powell County officials. And, as it turns out, Hall grew up in Powell county. Brooks is his brother in-law.
These were voices people in the area knew and trusted, the kind of voices Ingram said will resonate in other places.
Gamble, who runs the health department in Wheeling, said his department got a lot of support from health officials in nearby Pittsburgh and from West Virginia health departments such as Cabell-Huntington.
But every community has to make the decision to get on board. Watson hopes the work in Powell County can inspire other communities before it’s too late.
“Our community is not going to be here when our grandchildren come into this world, or when our great-grandchildren come into this world,” Watson said. “There’s not going to be anything left for them if we don’t take our community back.”
Based at WEKU, Richmond, Mary Meehan covers health for the ReSource. Reporter Alexandra Kanik contributed to this story.























The needle exchange program is the best thing to happen for addicts in so long I only wish the proram would come to people they a van or somewhere for people who can’t drive I have lived in Mount Sterling KY and they opposed not to get an exchange here for now and if it has been around b4 now maybe most of us addicts wouldn’t have Hep C